Tens of thousands of tonnes of extra medical waste from the response to the COVID-19 pandemic has put tremendous strain on health care waste management systems around the world, threatening human and environmental health and exposing a dire need to improve waste management practices, according to a new WHO report.
The WHO Global analysis of health care waste in the context of COVID-19: status, impacts and recommendations bases its estimates on the approximately 87,000 tonnes of personal protective equipment (PPE) that was procured between March 2020- November 2021 and shipped to support countries’ urgent COVID-19 response needs through a joint UN emergency initiative. Most of this equipment is expected to have ended up as waste.
The authors note that this just provides an initial indication of the scale of the COVID-19 waste problem. It does not take into account any of the COVID-19 commodities procured outside of the initiative, nor waste generated by the public like disposable medical masks.
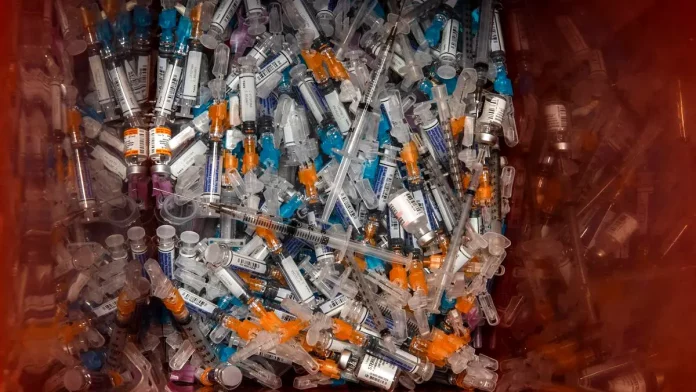
They point out that over 140 million test kits, with a potential to generate 2,600 tonnes of non-infectious waste (mainly plastic) and 731,000 litres of chemical waste (equivalent to one-third of an Olympic-size swimming pool) have been shipped, while over 8 billion doses of vaccine have been administered globally producing 144,000 tonnes of additional waste in the form of syringes, needles, and safety boxes.
As the UN and countries grappled with the immediate task of securing and quality-assuring supplies of PPE, less attention and resources were devoted to the safe and sustainable management of COVID-19 related health care waste.
Executive Director, WHO Health Emergencies Programme, Dr Michael Ryan said:
It is absolutely vital to provide health workers with the right PPE. But it is also vital to ensure that it can be used safely without impacting on the surrounding environment.
This means having effective management systems in place, including guidance for health workers on what to do with PPE and health commodities after they have been used.
Today, 30% of healthcare facilities (60% in the least developed countries) are not equipped to handle existing waste loads, let alone the additional COVID-19 load. This potentially exposes health workers to needle stick injuries, burns and pathogenic microorganisms, while also impacting communities living near poorly managed landfills and waste disposal sites through contaminated air from burning waste, poor water quality or disease carrying pests.
Director, Environment, Climate Change and Health at WHO, Dr Maria Neira said:
COVID-19 has forced the world to reckon with the gaps and neglected aspects of the waste stream and how we produce, use and discard of our health care resources, from cradle to grave. Significant change at all levels, from the global to the hospital floor, in how we manage the health care waste stream is a basic requirement of climate-smart health care systems, which many countries committed to at the recent UN Climate Change Conference, and, of course, a healthy recovery from COVID-19 and preparedness for other health emergencies in the future.
The report lays out a set of recommendations for integrating better, safer, and more environmentally sustainable waste practices into the current COVID-19 response and future pandemic preparedness efforts and highlights stories from countries and organizations that have put into practice in the spirit of “building back better”.
Recommendations include using eco-friendly packaging and shipping, safe and reusable PPE (e.g., gloves and medical masks), recyclable or biodegradable materials; investment in non-burn waste treatment technologies, such as autoclaves; reverse logistics to support centralized treatment and investments in the recycling sector to ensure materials, like plastics, can have a second life.
The COVID-19 waste challenge and increasing urgency to address environmental sustainability offer an opportunity to strengthen systems to safely and sustainably reduce and manage health care waste. This can be through strong national policies and regulations, regular monitoring and reporting and increased accountability, behaviour change support and workforce development, and increased budgets and financing.
Chair of the Health Care Waste Working Group, International Solid Waste Association,
Dr Anne Woolridge said:
A systemic change in how health care manages its waste would include greater and systematic scrutiny and better procurement practices. There is growing appreciation that health investments must consider environmental and climate implications, as well as a greater awareness of co-benefits of action. For example, safe and rational use of PPE will not only reduce environmental harm from waste, it will also save money, reduce potential supply shortages and further support infection prevention by changing behaviours.
The analysis comes at a time when the health sector is under increasing pressure to reduce its carbon footprint and minimize the amount of waste being sent to landfill — in part because of the great concern about the proliferation of plastic waste and its impacts on water, food systems and human and ecosystem health.