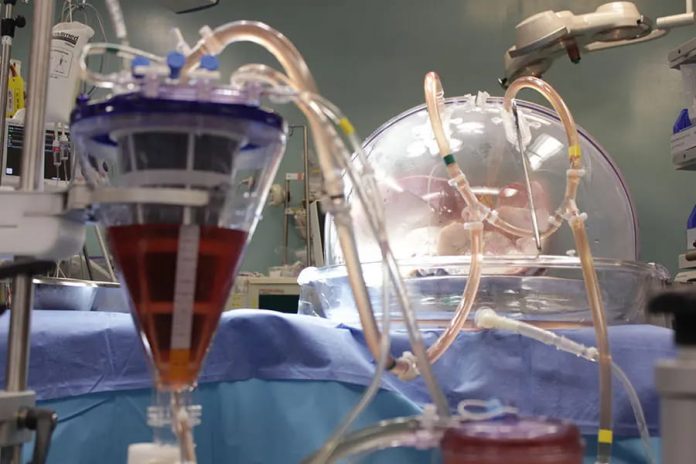
Ex vivo enzymatic treatment converts blood type A donor lungs into universal blood type lungs.
A study published in Science Translational Medicine performed at the Latner Thoracic Surgery Research Laboratories and UHN’s Ajmera Transplant Centre has proved that it is possible to convert blood type safely in donor organs intended for transplantation. This finding is an important step towards creating universal type O organs, which would significantly improve fairness in organ allocation and decrease mortality for patients in the waitlist.
Explains Dr. Marcelo Cypel, Surgical Director of the Ajmera Transplant Centre and the senior author of the study, who is also a thoracic surgeon at UHN’s Sprott Department of Surgery, a Professor in the Department of Surgery at the University of Toronto and the Canada Research Chair in Lung Transplantation.
With the current matching system, wait times can be considerably longer for patients who need a transplant depending on their blood type. Having universal organs means we could eliminate the blood-matching barrier and prioritize patients by medical urgency, saving more lives and wasting less organs.
Blood type is determined by the presence of antigens on the surface of red blood cells — type A blood has the A antigen; B has the B antigen; AB blood has both antigens; and O has none. Antigens can trigger an immune response if they are foreign to our bodies. That is why for blood transfusions we can only receive blood from donors with the same blood type as ours, or universal type O.
Likewise, antigens A and B are present on the surfaces of blood vessels in the body, including vessels in solid organs. If someone who is type O (meaning they have anti-A and anti-B antibodies in their bloodstream) received an organ from a type A donor, for example, the organ in all likelihood would be rejected. Consequently, donor organs are matched to potential recipients in the waitlist based on blood type, among other criteria.
Dr. Aizhou Wang, scientific associate at Dr. Cypel’s lab and first author of the study, explains.
Patients who are type O wait on average twice as long to receive a lung transplant compared to patients who are type A. This translates into mortality. Patients who are type O and need a lung transplant have a 20 per cent higher risk of dying while waiting for a matched organ to become available.If you convert all organs to universal type O, you can eliminate that barrier completely
This disparity is also present for other organs, she adds, where a patient who is type O or B in need of a kidney transplant will be on the waitlist for an average of four to five years, compared to two to three years for types A or AB.
The experiment
The experiment used the Ex Vivo Lung Perfusion (EVLP) System pioneered in Toronto as a platform for the treatment. The EVLP system pumps nourishing fluids through organs, enabling them to be warmed to body temperature, so that they can be repaired and improved before transplantation.
Human donor lungs not suitable for transplantation from type A donors were put in the EVLP circuit. One lung was treated with a group of enzymes to clear the antigens from the surface of the organ, while the other lung, from the same donor, remained untreated.
The team then tested each of the lungs by adding type O blood (with high concentrations of anti-A antibodies) to the circuit, to simulate an ABO-incompatible transplant. The results demonstrated that the treated lungs were well tolerated while the untreated ones showed signs of rejection.